Complete Guide to Gastric Sleeve Surgery
Gastric sleeve surgery is the leading bariatric procedure performed in North America. Gastric sleeve surgery boosts high expected-weight loss, low surgical-risks, and minimal side effects
Gastric sleeve surgery is one of many weight loss surgeries designed to help individuals lose weight. Gastric sleeve is a surgical procedure that helps weight loss by restricting food intake and reducing the hunger hormone Ghrelin. During this surgery, usually performed laparoscopically, 75-80% of the stomach is removed. This results in a sleeve or a tube shape stomach that holds much less food than prior to the surgery.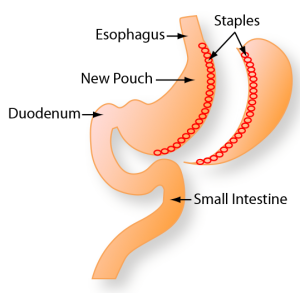 The gastric sleeve was created as the first stage of a two-stage procedure for high-risk (super obese patients. However, gastric sleeve surgery commonly is now used on its own for individuals with a body mass index (BMI) of over 40.
The gastric sleeve was created as the first stage of a two-stage procedure for high-risk (super obese patients. However, gastric sleeve surgery commonly is now used on its own for individuals with a body mass index (BMI) of over 40.
The average expected weight loss with the gastric sleeve procedure is typically 60% of the patient’s excess weight. Many individuals prefer the gastric sleeve surgery as there is no foreign object implanted into the body such as the gastric band. There also are no major changes in the intestines such as gastric bypass surgery. The procedure has a reasonable recovery and the procedure is permanent, unlike many other weight loss surgeries.
It’s important to understand why gastric sleeve is so successful. According to the University of Pittsburgh Medical Center, when you remove a portion of the stomach, the body’s level of ghrelin is reduced. Known as the “hunger hormone,” many individuals find their appetite is dramatically decreased after embarking on gastric sleeve surgery. Ghrelin is also a key component in blood sugar metabolism, so Type II Diabetics see an immediate decrease in their need for medication after gastric sleeve surgery. The American Society for Metabolic and Bariatric Surgery (ASMBS) reports that patients can expect improvements or even resolutions of a variety of medical conditions including (and not limited to): GERD, fatty liver disease, arthritis, sleep apnea, high blood pressure, high cholesterol, urinary incontinence, and asthma. Because of these improvements or resolutions, an improved quality of life can be expected after gastric sleeve surgery
Gastric Sleeve Surgery Candidacy
Determining whether one is eligible for gastric sleeve surgery will depend on many factors including their particular insurance. When consulting with a bariatric surgeon, they will be able to ensure that your insurance will accept you as a candidate for surgery and are well versed in working with different insurance companies.
In terms of general eligibility, the American Society for Metabolic and Bariatric Surgery generally follows two different types of candidates. The first is someone with a body mass index of over 40 or someone over 100 pounds overweight. The second is someone with a body mass index of over 35 and has at least two obesity-related co-morbidities. These comorbidities can include:
- Hypertension
- Sleep apnea
- Asthma and other respiratory disorders
- Type II Diabetes
- Osteoarthritis
- High cholesterol or lipid abnormalities
- GERD and other gastrointestinal disorders
- Non-alcoholic fatty liver disease
- Heart disease
The only other way someone can be eligible for this surgery is if they have not been able to experience healthy weight loss after a period of time.
The ASMBS, as well as the American College of Surgeons (ACS) and the NIH, all recommend that all weight loss surgeries including gastric sleeve surgery be performed by a board-certified surgeon with specializing training.
Risks & Complications Associated with Gastric Sleeve Surgery
Gastric sleeve surgery has a high survival rate of 99.7%. However, according to the U.S. National Library of Medicine, there are some risks and complications associated with the surgical procedure. Some of the most common include bleeding, stenosis and staple line leaks and infection. Blood clots are a common concern with any type of surgery, that’s why your surgeon will require you walk around as soon as possible after surgery and wear compression stockings.
There are also some side effects that are common in those that have gastric sleeve surgery that is less as serious. These include digestive issues, gallstones (from excessive weight loss), nausea and vomiting as well as vitamin and mineral deficiency. The latter should be addressed appropriately with a post-op vitamin regimen.
In some cases, patients manage sagging skin with body-contouring undergarments. In more serious cases, patients have plastic surgery to remove the excess skin. Surgery to remove excess skin is often covered by insurance.
Before Gastric Sleeve
Your surgeon will work closely with you during the time leading up to your gastric sleeve surgery. Your health assessment will include asking you questions about your medical history, surgical history as well as any medications you take. A variety of tests may be ordered including x-ray, blood tests or an ECG.
You will also need to establish a pre-surgery diet regimen. The two weeks before you cannot have any sugar. Your diet will be lower carb, increased protein and veggie and lots of fluids. Two days before your surgery, you will have only clear liquids, broth, and just one protein shake daily. 12 hours before surgery, you cannot eat or drink or smoke.
Ultimately the main goal before surgery is to lose as much weight as possible. The lower that your pre-op surgery is, the lower your risk of complications are.
During Surgery
According to NIH, your surgeon will remove 75-80% of your stomach, which leaves a sleeve that connects your esophagus to the small intestines. This will cause you to feel full sooner and result in long-term weight loss. This surgery is typically done laparoscopically and takes about 1 to 2 hours. You will be under general anesthesia during surgery.
Expected Excess Weight Loss with Gastric Sleeve Surgery
Weight loss will be relative to each patient and their original weight, their existing and post-op medical history as well as their dedication to their new lifestyle including diet and regular exercise. Weight loss does happen fast after gastric sleeve surgery. There have been countless studies published on gastric sleeve weight loss with a large range of expectations set forth for patients. One study by Gagner et al complied weight loss data from nearly 46,133 operations and 130 different surgeons. They found that average gastric sleeve weight loss was about 55-59% of excess weight loss from one to three years post-op.
Overall, the industry average sees about 1/3 of excess weight loss by month 3, half of the excess weight loss by 6 months post-op and about 70% of weight gone in one year. Another astounding statistic comes from The New England Journal of Medicine who reports that gastric sleeve surgery resulted in 23-40% reduction of premature mortality because of obesity or comorbidity related to a patient’s weight.
Post-Op and After Gastric Sleeve
Gastric sleeve patients usually stay in the hospital for a few days following their weight loss surgery. Full recovery generally occurs in about six weeks. After you wake up from surgery, you will feel sore and out of it. Your surgeon will want you to move as soon as possible as this reduces the risk of blood clots and jumpstarts the healing process.
Before you are released from the hospital you will be required to:
- Walk
- Drink enough to stay hydrated without vomiting
- Urinate yourself after your catheter is removed
- Can feel relief from pain with pain medication (no IV medication)
According to ASMBS, it’s important that you contact your surgeon immediately if you experience ongoing nausea or vomiting, no improvement or worsening of pain, signs of incision infection, fever or difficulty swallowing.
You will have follow-ups regularly at one-week post-op, four-week post-op and every several months after that point.
Diet After Gastric Sleeve
Following the post-op diet is important for one’s success with weight loss. The University of Michigan Health System offers helpful tips on what diet to follow following your surgery.
When you arrive home, you will be on a liquid diet for 2 weeks. You will need to sip small amounts of fluids or have small spoonfuls of liquids throughout the entire day. You need a minimum of 64 ounces of decaf fluids daily to stay hydrated. In terms of protein, your goal will be 70 grams a day.
Do not advance yourself to the next phase of diet until you consult your surgeon.
Some fluids or foods allowed in liquid phase include:
- Cream of wheat or cream of rice cereal (no oatmeal) made with skim/ low-fat milk
- Mashed potatoes – made with skim/ low-fat milk
- No-sugar-added pudding
- No-sugar-added yogurts
- Beef, chicken or vegetable broth
- No-sugar-added popsicles, fruit bars or fudge bars
- Tomato juice (no v-8 splash)
- Sugar-free Jell-O
- Any skim or low-fat milk
- Decaf/herbal tea or decaf coffee
- No-sugar-added high-protein supplement
- Non-caffeinated, non-carbonated, calorie-free water or beverages
The next step is the pureed diet, which you will be on for 2 weeks following your liquid diet. Everything must be pureed to baby food consistency. You may have all the foods listed above as well as:
- Oatmeal
- Soft, lean meats
- Eggs/egg whites
- Frozen or canned vegetables, very cooked (No raw veggies until six weeks post-op)
- Canned fruits in water (no syrup)
- No-sugar-added applesauce
- Beans
- Chili
- Soups
- Low-fat soft cheeses
- Baby food
Things to avoid: Rice, pasta, crackers, and bread.
Your final diet is a soft diet for 4 weeks. Follow all the foods from the pureed diets, but you don’t have to puree anymore. This is a low-fat and no-sugar-added diet. The goal here is to eat small amounts of food every three to four hours. Aim for four to six meals a day. Drink at least 64 ounces of water daily. Never drink with meals throughout the entire post-op diet (pureed and soft foods).
Vitamins & Supplements
As a part of your post-op diet, you should take a series of supplements to feel your best. You will take a multivitamin, calcium for your bones, folate for your blood, iron for your blood and Vitamin D for your overall health.
How to Maximize Weight Loss with Gastric Sleeve
First and foremost, you must follow a low-fat diet to see success. On top of following this diet, you must exercise regularly. Many studies show that patients who exercise regularly lose more weight over the long term. Choose from a variety of exercises whether endurance, flexibility or strength training. Some popular endurance activities include walking, swimming and the stationary bike. Yoga is a great stretching supplement to regular activity. Lastly, strength training includes weights, which helps to tone sagging skin that many patients experience after excess weight loss following their weight loss surgery.
In terms of other tips to maximize weight loss after surgery, the NIH offers some suggestions that have proven results.
- Don’t drink your calories. Your caloric intake is limited and that is so you lose weight. Don’t work against yourself and slow your weight loss by doing this unhealthy habit.
- Stop snacking. This habit can slow progress. Avoid junk foods and eat high-quality meals regularly (every several hours).
- Up your protein intake. This should be your primary focus. It helps maintain muscle mass while losing fat and helps you to feel full longer in between meals.
- Skip alcohol. Ultimately it is just full of empty calories that provide no nutrition to you. It can also contribute to ulcers, which you already are at risk for after surgery.
- Find a support group. These support groups are a great place to talk to people who understand what you’re going through and who can offer you suggestions of new things to try throughout your journey. Here you can also learn helpful coping skills to get over your food addiction.
- Listen to your body closely. Don’t eat when you aren’t hungry. Instead, drink a glass of water before you do.
- Avoid simple carbs. These highly-processed foods can stall your weight loss journey. They also elevate blood sugar, which increases cravings. Focus on whole foods.
- Stay hydrated. Drink lots of water as it will keep you feeling full and help your body function at its best.
More Resources for Gastric Sleeve Surgery
- Costs of Gastric Sleeve Surgery
- Life and Recovery of Gastric Sleeve Surgery
References
- http://columbiasurgery.org/conditions-and-treatments/sleeve-gastrectomy
- http://www.upmc.com/services/bariatrics/approach/surgery-options/pages/gastric-sleeve.aspx
- https://asmbs.org/patients/benefits-of-bariatric-surgery
- https://asmbs.org/patients/who-is-a-candidate-for-bariatric-surgery
- http://www.mayoclinic.org/tests-procedures/bariatric-surgery/basics/risks/prc-20019138
- https://www.niddk.nih.gov/health-information/health-topics/weight-control/bariatric-surgery/Pages/types.aspx
- https://www.ucsfhealth.org/education/recovering_from_bariatric_surgery/
- http://www.med.umich.edu/bariatricsurgery/resources/Post-op-Diet-Sleeve.pdf
- https://health.ucsd.edu/specialties/surgery/bariatric/weight-loss-surgery/Pages/comparison-chart.aspx
- https://www.move.va.gov/docs/moveReferenceManual/11_BariatricSurgery.pdf