Complete Guide to Gastric Bypass Surgery
Gastric bypass surgery is a weight loss surgery procedure where the stomach itself is divided into an upper and lower pouch.
Gastric sleeve surgery is one of many weight loss operations designed to help individuals lose weight. Gastric sleeve is a surgical procedure that promotes weight loss by restricting food intake and reducing the hunger hormone Ghrelin. During this surgery, usually performed laparoscopically, 75-80% of the stomach is removed. This results in a sleeve or a tube shape stomach that holds much less food than before the surgery.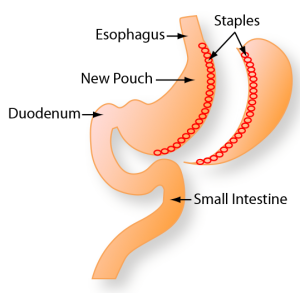
The small stomach pouch is typically out an ounce in size. After the bariatric surgeon makes that division, the small intestine is rearranged so that it can connect both of these pouches. It is moved down further in the body so that digestive enzymes and stomach acids will eventually mix with the food. This helps to restrict the amount of food that the patient can consume. This leads to weight loss. Also, there is less digestion of food because of this smaller stomach pouch. Because the small intestine would typically absorb calories and nutrients, there is a less absorption of both with this bypass. The rerouting process produces important changes in the gut hormones (for instance, ghrelin, the hunger hormone) that helps to suppress hunger and to reverse some of the things that produce medical conditions such as Type II Diabetes. Ultimately, there are a few ways to reconnect the intestine leading to different types of gastric bypass surgery and a surgeon can determine the most effective surgical technique for your gastric bypass surgery.
The surgery itself is done to help treat morbid obesity (for individuals with a body mass index of 40 or more) and as a way to help treat comorbidity such as obstructive sleep apnea, Type II Diabetes or high blood pressure (for individuals with a BMI of 35 or more). As with any other surgery, it’s not uncommon for some complications to occur, however according to many recent studies, only about 15% of patients experience any at all, and severe ones occur in less than 3% of patients.
Types of Gastric Bypass Surgeries
The first variation is Roux-en-Y. During this surgery type, the small intestine is divided below the lower stomach into a Y shape that allows food to flow from the upper stomach pouch (described above). The Y intersection created by a bariatric surgeon is made at the end of the small intestine. The Roux limb is made from portions of the small intestine, which allows the body to absorb nutrients. Patients will feel full quickly and later have an indifference to food after they start to eat.
Another type is the mini gastric bypass surgery. During this procedure, a long and narrow tube in the stomach is made from a loop of a portion of the gut. This loop is then later hooked into this tube at the beginning of the small intestine. Often this bariatric surgery is used to treat stomach injuries, ulcers, and even stomach cancer. It is considered an alternative to Roux-en-Y because of the way the operation is constructed. It is becoming one of the most popular bariatric surgeries because it has a low risk of complications with patients seeing the same steady weight loss as other weight loss surgeries.
Do I Qualify for Weight Loss Surgery?
Research has proven that all types of weight loss surgery can benefit individuals with body mass indexes (BMIs) of 35-39.9 with comorbidities. These comorbidities are obesity-related health conditions and can include and are not limited to: high blood pressure, high cholesterol, breathing problems, obstructive sleep apnea and Type II Diabetes, just to name a few.
Ultimately requirements will vary on the type of weight loss surgery and the surgeon you choose, a person is generally a weight loss surgery candidate if they are more than 100 pounds over their ideal weight, they have comorbidities (as mentioned above) and are unable to achieve a healthy body weight on their own even with medically-supervised dieting. To qualify, individuals must be willing to commit to their new healthy and active lifestyle. They shouldn’t have any medical issues that can put them at risk for any severe surgery complications.
According to the American Society for Metabolic and Bariatric Surgery (ASMBS), the National Institute of Health and the American College of Surgeons (ACS), all surgeries should be performed by a board-certified surgeon with specialized training in both bariatric and metabolic surgery for the most success. Also, some insurance companies require that the weight loss surgery is performed at a facility that meets the ASMBS-approved quality standards. Mayo Clinic reports that in some rare cases, a patient may qualify for weight loss surgery with a BMI of 30 to 34 with some weight-related severe health problems.
During an initial consultation with a weight loss surgeon, it will be determined whether or not you are a candidate for the procedure you have chosen and for your insurance (both may have different requirements).
Expected Excess Weight Loss with Gastric Bypass Surgery
It is normal for a patient to be curious about how much weight they can expect to lose when choosing to undergo gastric bypass surgery. Ultimately, knowing how much weight you can expect to lose is an essential part of setting goals for yourself and your future. Weight loss is guaranteed with a weight loss surgery procedure such as gastric bypass, but not the amount of weight itself. The amount of pressure that is lost after gastric bypass will be determined by both the success of the surgery and one’s nutrition and exercise plan following surgery. Making lifestyle changes is essential for continued weight loss for weight loss surgery patients, no matter what surgery type they choose.
Most patients can expect to lose between 65-70% of their excess weight with gastric bypass surgery alone. It’s important to understand the critical difference between one’s starting weight and their excess weight. You won’t lose 70% of your starting weight, but the amount of weight you want to lose (70% of that). The actual weight loss seen will be distinct to each patient, they report.
For example, if a patient is 250 pounds and 104.4 of that is excess weight, 65% weight loss would be equivalent to about 68 pounds. For someone who is 400 pounds with approximately 205.3 pounds of excess weight, weight loss would be about 133 pounds lost. As you can see with these examples, the numbers themselves can vary, but the percentage of weight loss remains about the same.
During a U.S. National Library of Medicine National Institutes of Health 15-year study on gastric bypass patients, they found that long-term weight loss success is achievable. Their study evaluated patient’s outcomes after an extended period (sometimes ten years later) to see how much patients lost after surgery. The study evaluated about 3,227 patients who all had gastric bypass surgery with an average BMI of 43. The study found that after 15 years, 47.1% of all excess weight loss was maintained.
While these statistics show a high success rate, it’s important to note that when you’re looking at these expected weight loss studies that you look at how much of that weight loss was maintained over an extended period. Keeping the weight loss is what allows these patients to maintain their health over a lifetime.
Patients typically lose about half or so of their excess weight in the first two years following their gastric bypass surgery. Weight loss plateaus do occur, and if one happens for more than six weeks, it’s important to see your doctor, so they can make adequate changes to your diet and exercise routine to restart your weight loss. Also, it is common for someone to regain a small portion of their weight before their weight stabilizes. This is because the new body is readjusting to its original form and gravity in general.
What to Expect With Gastric Bypass Surgery
Being prepared for what to expect before, during and after gastric bypass allows patients the most excellent chance of success overall. A weight loss surgeon will be able to answer any questions related to this process along the way so that a patient is comfortable and knowledgeable about the process. For instance, understanding the risks associated with weight loss surgery is essential. Some risks associated with gastric bypass surgery include stomach pouch problems (requiring a repeat surgery), hernia, kidney stones or gallstones.
Pre-Op Surgery
To prepare for gastric bypass surgery, a series of tests must be done. According to the University of Iowa Hospital, these may include a complete blood count, urinalysis, and a chemistry panel as well as a chest x-ray and an electrocardiogram. In weight loss surgery cases, some surgeons require a gallbladder ultrasound to look for gallstones. Other tests such as sleep studies, GI evaluation or psychiatric evaluation may be necessary. Ultimately, what is expected of you, will depend on your surgeon and your insurer. A GI evaluation is essential especially with those with significant gastrointestinal symptoms to look for ulcers or hiatal hernias before surgery.
If you smoke, you must stop before surgery. Also, a pre-op liquid diet will be required for an undisclosed period to prepare the body for surgery and nutritional changes.
During Surgery
According to the U.S. National Library of Medicine, gastric bypass surgery can take from two to four hours. A surgeon will make small incisions into the abdomen where scope and instruments are inserted. A camera is connected to a video monitor in the operating room allowing the weight loss surgeon to view inside the belly while they perform the surgery. A laparoscopy means less pain, shorter hospital stay and most importantly, a quicker recovery for patients.
Diet and Life After Gastric Bypass
Most gastric bypass patients spend three to five days in the hospital following surgery. While there, you will be asked to sit on the side of the bed and to walk a little on the day of their operation. You may have a catheter from their nose into the stomach for a few days that helps to drain fluids. You will not be able to eat for a few days aside for liquids. You must wear support stocking to help prevent blood clots. Most often, you will receive your medication through shots or IV. You will be able to go home once you can eat liquid and pureed food without vomiting, you can move around with ease and without a lot of pain and no longer need IV pain medication.
It is normal to have pain for at least the first week following gastric bypass surgery. Your incisions may feel sore or tender. You will feel full faster and may have digestive problems as your body adjusted to the new re-routing internally. Always follow all of the post-op instructions given to you by your surgeon following surgery. For the first month after surgery, your stomach will only be able to handle a small amount of food at a time. This means you must stay hydrated throughout the day, not only to help your body digest but to feel well. You will need to take supplements such as B12, iron, magnesium, calcium and other vitamins. You should be able to return to work after four to six weeks, the University of California, San Francisco reports.
Regarding a post-op diet, patients go through several stages including liquids, soft foods and then solids. During the bright liquid stage, which usually occurs for one to two days after surgery, patients can have sugar free juice, water, broth, flat diet soda and diet gelatin, just two to three ounces at a time. If they have no issues, they move onto high-protein liquids such as Ensure for one to two weeks. After that, the soft/pureed foot diet is introduced with foods such as low-fat cheese, blended tuna, scrambled eggs or cottage cheese. About two months after bypass surgery, a regular menu is enjoyed. Patients must have several small meals a day and eat ½ cup of food at a time to prevent dumping syndrome symptoms from occurring.
How to Maximize Weight Loss with Gastric Bypass Surgery
Adjusting to your new diet and lifestyle can be difficult. However, by taking the time to learn helpful tips to maximize your weight loss, your surgery will become more of success over time.
In terms of nutrition, avoid sugar. Sugar is empty calories and causes hunger to strike out of nowhere. Also, don’t drink your calories. Your caloric intake will be limited both after surgery and in order to lose weight. Make every calorie count by focusing on fruits and vegetables and protein first. Also, avoid carbonated drinks as the bubbly nature may cause increased pressure on the stomach leading to pain or discomfort. It’s also important to limit liquids before, during or after meals. There is a small amount of space reserved for food now after surgery, so drinking during these times will wash food out of your stomach, making you feel hungry sooner. Try not to snack, this can slow your progress. If you’re hungry, just have a small meal (you should be having up to six a day). Chewing your food also is important not only to keep you full, but for digestion, which must adjust for a period of time following gastric bypass surgery.
In terms of follow-up visit, visit your surgeon so that your progress can be closely monitored. Also, don’t stop taking any medications without your surgeon’s approval first. In saying that, don’t take any over-the-counter drugs without approval either as they can increase your chance of ulcer or constipation. A surgeon also will suggest support groups. It’s important to surround yourself around those who have already walked this journey and who can offer helpful tips for you to succeed.
Conclusion
Remember that gastric bypass or any weight loss surgery won’t fix your life. It is not a miracle fix, but it is meant to help you get healthier. For those who have used food for a coping mechanism, it’s important that new coping skills are learned to prevent this negative behavior from occurring. Ultimately, gastric bypass surgery gives you the chance to work hard in order to restore your health. Good luck on your journey to optimal health!
- Costs of Gastric Bypass Surgery
- Life and Recovery of Gastric Bypass Surgery
- Pre-Operative Gastric Bypass Diet
- Post-Operative Gastric Bypass Diet
References
- https://asmbs.org/patients/bariatric-surgery-procedures
- http://www.mayoclinic.org/tests-procedures/bariatric-surgery/in-depth/weight-loss-surgery/art-20045334
- https://asmbs.org/patients/who-is-a-candidate-for-ebariatric-surgery
- http://www.mayoclinic.org/healthy-lifestyle/weight-loss/in-depth/gastric-bypass-surgery/art-20046318
- https://uihc.org/health-library/pre-operative-obesity-surgery-faqs
- https://medlineplus.gov/ency/article/007199.htm
- https://www.ucsfhealth.org/education/recovering_from_bariatric_surgery/